Shoulder surgery can be a turning point. For many patients, it offers a path back to daily activities they thought they had lost. But like any surgical procedure, it comes with potential complications. Understanding potential shoulder surgery problems before you head into the operating room may help you make more informed decisions.
Whether you are considering a total shoulder replacement, a reverse shoulder replacement, or a repair procedure, taking a proactive approach can make a meaningful difference. In this post, we explore the most common shoulder surgery problems patients encounter, what you can do to help minimize your risk, and how advances in implant technology are aiming to improve long-term outcomes for shoulder replacement patients.
Key Takeaways
- Shoulder surgery problems can range from infection and stiffness to implant loosening.
- Glenoid loosening remains one of the most common reasons patients require revision surgery after a total shoulder replacement. Newer implant designs aim to address this issue by improving fixation and mechanical stability.
- Patient involvement in rehabilitation and following post-operative instructions plays a role in long-term success.
What Are the Most Common Shoulder Surgery Problems?
No surgical procedure is without risk. The likelihood of issues depends on several factors, including your overall health, the type of procedure, and how well post-operative care guidelines are followed. Some of the more frequently reported shoulder surgery problems include the following:
Infection
Infections can occur after any procedure. An infection may require additional surgery, extended antibiotic treatment, or in some cases, implant removal. Your surgical team typically takes preventive measures such as maintaining strict sterile protocols.
Stiffness and Frozen Shoulder
Post-surgical stiffness is one of the more common shoulder surgery problems patients experience. If the shoulder joint does not regain its range of motion after surgery, a condition sometimes called frozen shoulder or adhesive capsulitis may develop. This can make even basic tasks feel difficult. Physical therapy usually plays a role in preventing stiffness. Starting rehabilitation as directed by your surgeon and staying consistent with your exercises may help reduce your chances of developing this complication.
Nerve or Blood Vessel Damage
During any shoulder procedure, nerves and blood vessels near the surgical site face some degree of risk. While permanent damage is uncommon, temporary numbness or tingling can occur.
Blood Clots
Though more common in lower extremity surgeries, blood clots can form after shoulder procedures as well. Reduced mobility during recovery may increase this risk. Early mobilization and following your surgeon’s post-operative instructions may help reduce the likelihood of clot formation.
Implant-Related Complications
For patients receiving a shoulder replacement, implant-related complications represent some of the most common shoulder surgery problems. These can include implant loosening, component wear, instability, or dislocation. Among these, glenoid component loosening has historically been one of the leading concerns in total shoulder arthroplasty.
The Glenoid Loosening Challenge in Total Shoulder Replacement
Total shoulder replacement surgery, also known as total shoulder arthroplasty, involves replacing both the ball and the socket of the shoulder joint with artificial components. The procedure has helped relieve pain and restore function in many patients over the years. However, glenoid loosening has remained a persistent challenge.
The glenoid component is the part of the implant that replaces the socket side of the shoulder joint. Over time, mechanical stresses can cause this component to shift or loosen from the underlying bone. When that happens, patients may experience renewed pain, reduced function, and potentially the need for revision surgery.
Traditional glenoid implant designs have often sat on the surface of the bone. This approach can sometimes leave the component more vulnerable to what orthopedic professionals refer to as “rocking horse” forces. These repetitive, back-and-forth stresses at the bone-implant interface may gradually compromise the fixation, leading to loosening.

Glenoid loosening represents one of the most frequently cited reasons patients undergo revision shoulder surgery. It does not happen overnight. Rather, it tends to develop gradually over months or years. That said, advances in implant design are working to address this concern more effectively than ever.
How Modern Implant Technology Aims to Address Glenoid Loosening
As orthopedic technology has evolved, implant manufacturers have focused more attention on improving glenoid fixation. One of the more notable innovations in this space comes from Shoulder Innovations and their InSet® Glenoid component.
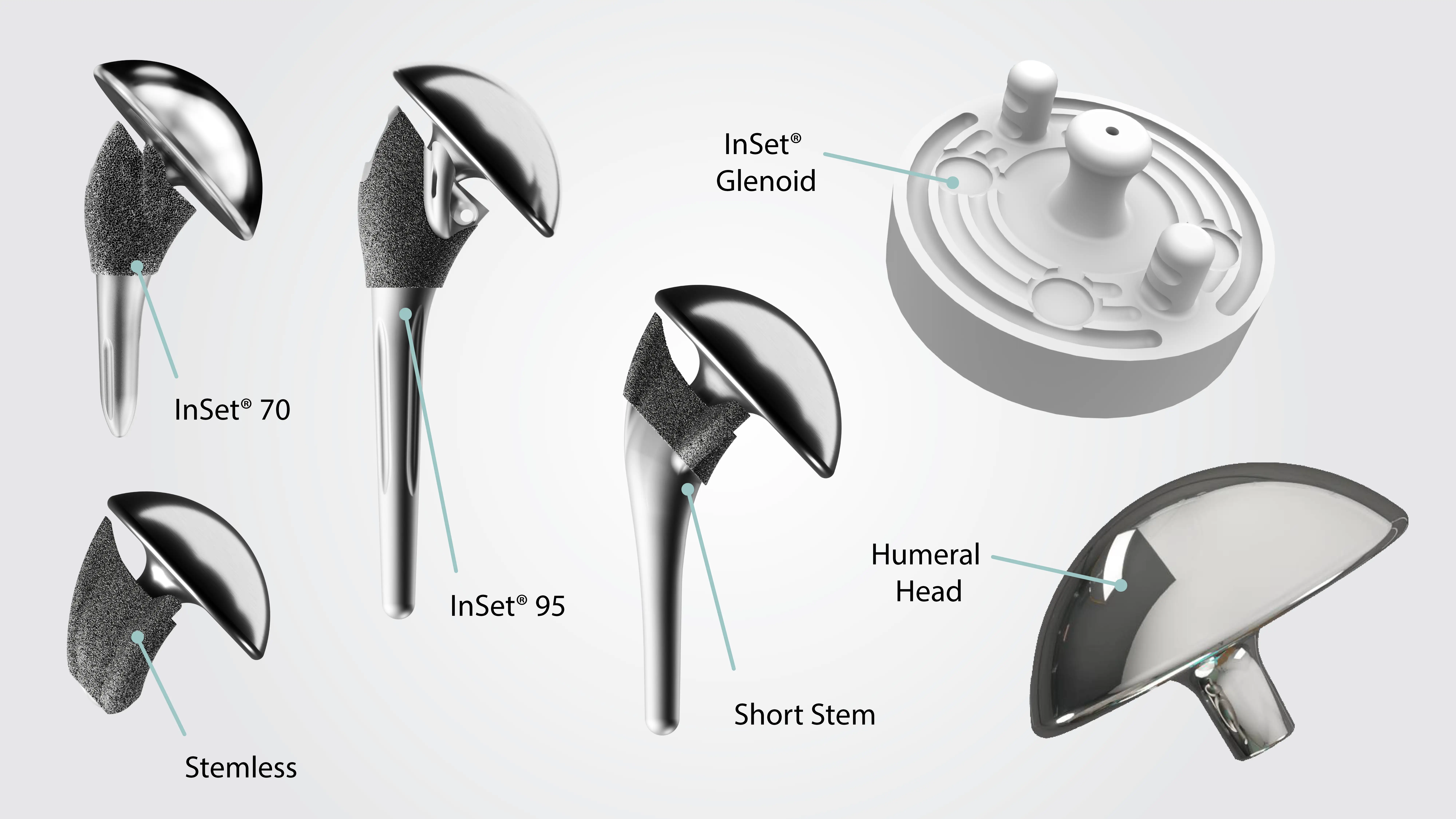
The InSet® Glenoid takes a fundamentally different approach to how the socket component is placed. Rather than sitting on top of the bone surface, the InSet® design positions the implant within a pocket of sclerotic bone. Sclerotic bone is the denser, harder bone that exists just beneath the joint surface. By seating the implant within this stronger bone, the design aims to create a more mechanically stable foundation.
Finite Element Analysis modeling has demonstrated that the InSet® Glenoid design may reduce the “rocking horse” stresses associated with loosening by as much as 87% in simulated conditions. In my practice, I prioritize implant designs that aim to enhance fixation and reduce mechanical stress, which is why I incorporate this system into my surgical approach.
The system also offers multiple implant options, including short stem and stemless humeral components, as well as augmented glenoid options for patients with bone loss. Additionally, the ProVoyance® planning software can be used to optimize implant fit in three dimensions, tailoring the procedure to each patient’s unique anatomy.
For patients considering total shoulder replacement, asking your surgeon about the implant system they use and how it addresses glenoid loosening is a worthwhile conversation. Not all implant designs approach this problem the same way, and understanding the differences may help you feel more confident about your care plan.
How Choosing the Right Surgeon May Help You Avoid Shoulder Surgery Problems
Your choice of surgeon is one of the most important decisions you can make. A fellowship-trained shoulder surgeon brings specialized expertise. Fellowship training in the shoulder involves additional education beyond residency, specifically focused on the shoulder joint and its complexities.
Surgeons with focused training in shoulder procedures may have additional experience managing complex shoulder conditions and may stay current with evolving research and technology, which can influence surgical planning and decision-making.
When you meet with a prospective surgeon, consider asking these types of questions:
- Are you fellowship-trained in shoulder surgery?
- What is your approach to managing surgery complications?
- What does your typical rehabilitation plan look like after surgery?
- How many shoulder replacements do you perform each year?
Steps You Can Take to Help Minimize Shoulder Surgery Problems
While your surgeon handles the technical aspects of your procedure, you play a role in your own outcome. Preparation and commitment to recovery can make a real difference.
Prepare Your Body Before Surgery
Your overall health at the time of surgery can influence your results. If you smoke, quitting before your procedure may reduce your risk of infection and improve healing. Managing chronic conditions like diabetes is also important. Ask your surgeon if there are specific exercises or lifestyle changes you should make in the weeks leading up to surgery.
Commit to Your Rehabilitation Plan
Physical therapy after shoulder surgery is often a core part of your recovery. Your therapist will guide you through exercises designed to restore range of motion, rebuild strength, and help you regain function. Consistency is key.
Follow Post-Operative Instructions Carefully
Your surgeon will provide detailed guidelines about activity restrictions, wound care, medication management, and when to follow up. Ignoring weight-bearing restrictions or returning to activities too soon can compromise your results and increase the risk of complications.
Frequently Asked Questions
What are the most common shoulder surgery problems after a total shoulder replacement?
The most frequently reported complications after total shoulder replacement tend to include infection, stiffness, nerve irritation, and implant-related issues such as glenoid loosening or instability. Many of these risks may be reduced through careful surgical technique, thoughtful implant selection, and a strong commitment to post-operative rehabilitation.
What is glenoid loosening and why does it matter?
Glenoid loosening occurs when the socket-side component of a total shoulder replacement shifts or separates from the underlying bone over time. It is considered one of the leading causes of implant failure in total shoulder arthroplasty. When loosening occurs, patients may experience pain and loss of function, which can lead to the need for revision surgery.
How long does it take to recover from shoulder replacement surgery?
Recovery timelines vary from patient to patient. Many individuals begin to notice meaningful improvement within the first several weeks to months after surgery. However, full recovery may take up to a year or longer. Your surgeon will create a personalized rehabilitation plan based on your specific procedure and condition.