When the structures that keep the ball of the upper arm bone (humerus) centered in the socket (glenoid) are compromised, the shoulder can become loose or unstable. This condition, known as shoulder instability, can range from a subtle feeling of looseness to a complete dislocation. Understanding the causes of shoulder instability is a key step toward effective diagnosis and treatment.
Key Takeaways
- The shoulder’s stability relies on a delicate balance of static restraints (bone, labrum, capsule, ligaments) and dynamic restraints (muscles and tendons).
- Instability can be broadly classified as traumatic (injury-related) or atraumatic (non-injury related).
- A thorough evaluation is important to determine the specific cause and tailor the most appropriate treatment plan.
The Anatomy of a Stable Shoulder
To understand the causes of shoulder instability, it is helpful to first understand how a healthy shoulder maintains its stability. The shoulder is a ball-and-socket joint, but the socket is quite shallow, resembling a golf ball on a tee. This design allows for extensive movement but requires several supporting structures to keep the joint secure.
Static Stabilizers
These structures provide passive stability and do not require muscle contraction to function.
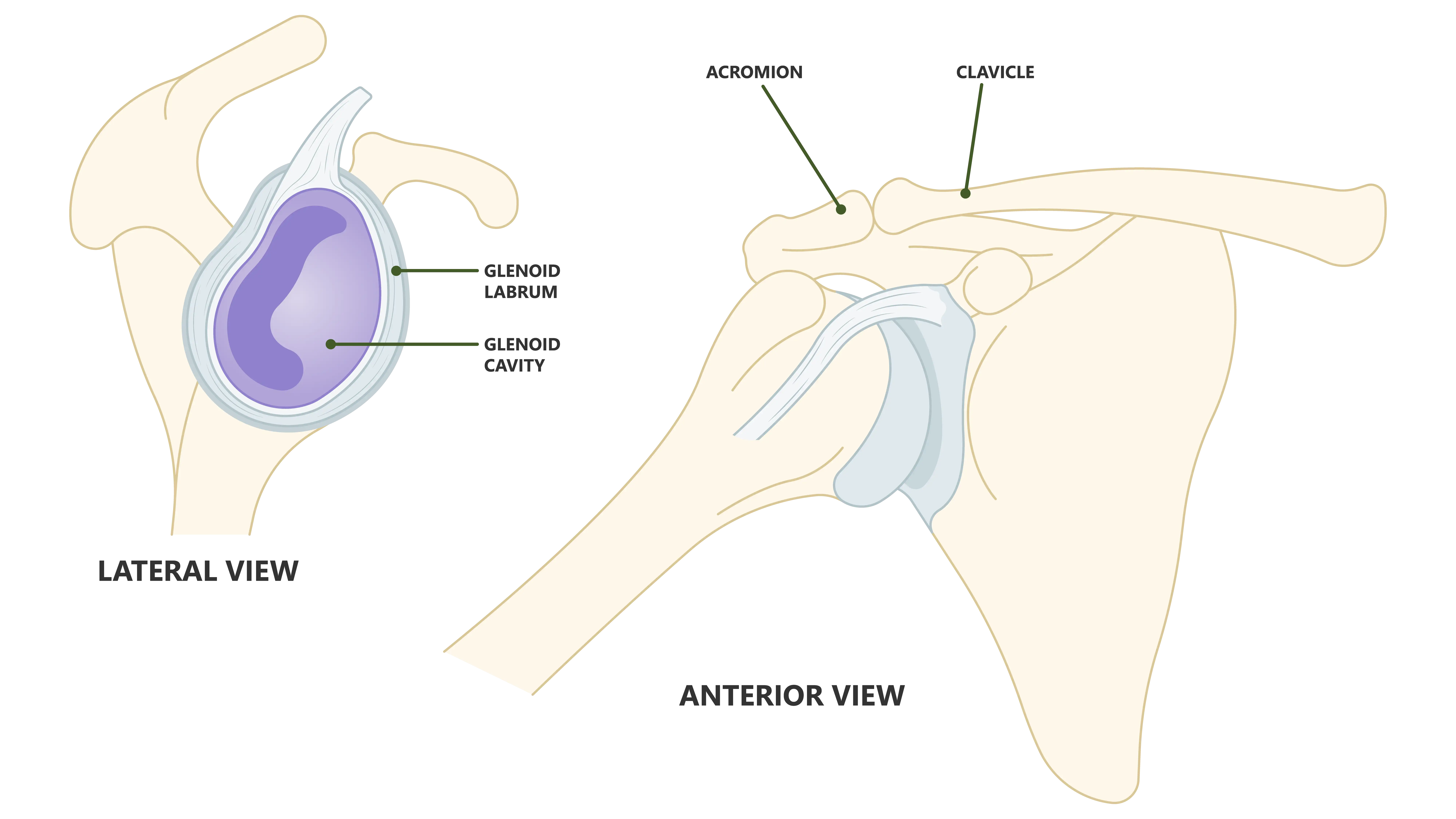
- The Glenoid Labrum: This is a ring of fibrocartilage that encircles the glenoid socket. It deepens the socket, creating a more secure fit for the humeral head.
- The Joint Capsule and Ligaments: The capsule is a fibrous sac that encloses the joint. Thickened bands within the capsule form the glenohumeral ligaments, which act like strong ropes to hold the ball in place, especially at the extremes of motion.
- Bony Congruity: The shape of the humeral head and the glenoid socket contribute to stability.
Dynamic Stabilizers
These structures provide active stability through muscle contraction. They are particularly important during movement and when the arm is under load.
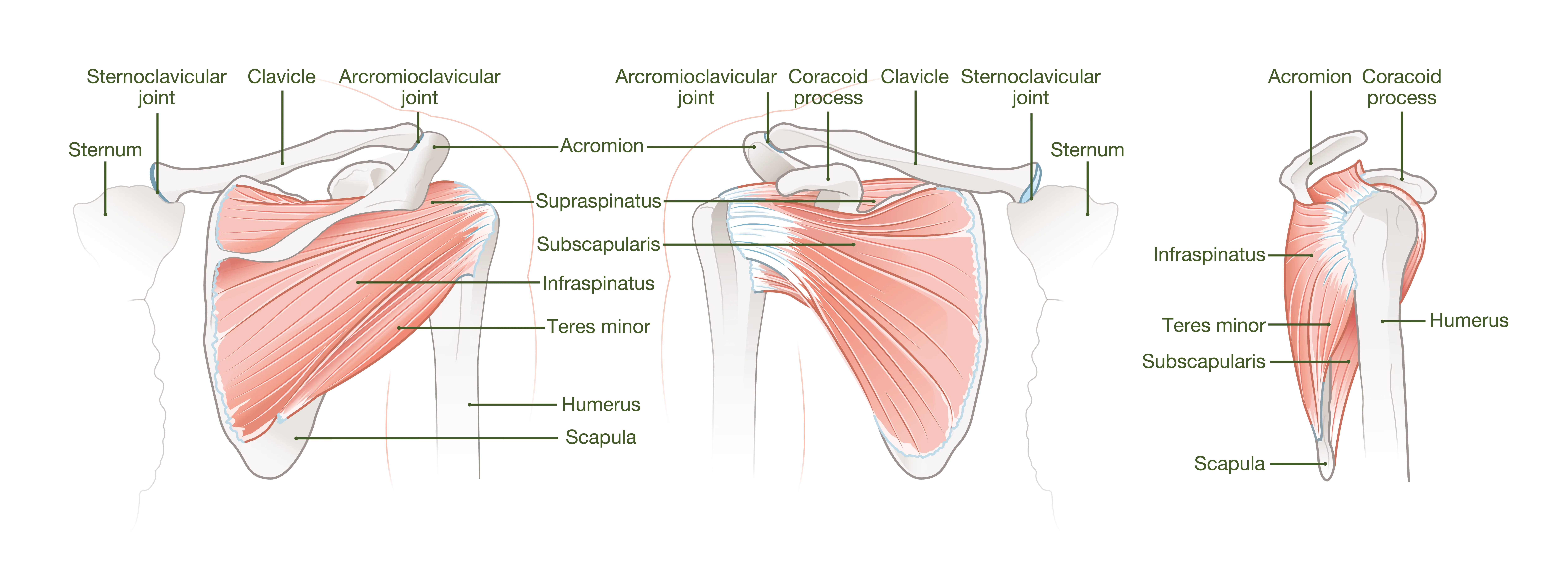
- The Rotator Cuff Muscles: This group of four muscles (supraspinatus, infraspinatus, teres minor, and subscapularis) surrounds the joint. They work together to keep the humeral head centered in the glenoid during arm movement.
- The Scapular Stabilizers: Muscles like the serratus anterior and trapezius control the movement and position of the shoulder blade (scapula).
Categorizing the Causes of Shoulder Instability
Orthopedic specialists often classify shoulder instability based on its origin, which can help guide the treatment approach. The two primary categories are traumatic and atraumatic instability.
1. Traumatic Instability
Traumatic instability is the most common form. It occurs when a significant, forceful event causes the shoulder to dislocate or partially dislocate (subluxate). This is often a sudden, painful injury. The typical mechanism involves a fall onto an outstretched arm or a forceful blow to the shoulder when the arm is abducted (raised away from the body) and externally rotated.
Key Structural Injuries
When the force is strong enough to cause a shoulder dislocation, it may damage the static stabilizers.
- Bankart Lesion: This is the most frequent injury associated with traumatic anterior dislocation. It is a tear of the anterior-inferior labrum, where the labrum is pulled off the front rim of the glenoid. This tear reduces the depth of the socket.
- Bony Bankart Lesion: In some cases, the force is so great that it tears a piece of bone along with the labrum.
- Hill-Sachs Lesion: As the humeral head dislocates, it can impact the front edge of the glenoid. This impact creates a compression fracture, or dent, on the back and upper part of the humeral head.
- Capsular and Ligamentous Tears: The glenohumeral ligaments and the joint capsule are stretched or torn during the dislocation. Once stretched, these tissues may not heal back to their original tightness, leaving the joint loose.
2. Atraumatic Instability
Atraumatic instability occurs without a single, significant injury. Instead, it often develops gradually due to repetitive stress or an underlying anatomical predisposition. Repetitive microtrauma is a common cause in athletes who perform frequent overhead motions, such as baseball pitchers, swimmers, and volleyball players. The repeated, high-velocity movements can gradually stretch the joint capsule and ligaments over time.
Some individuals are naturally “double-jointed” or have a genetic predisposition for loose ligaments throughout their body. This condition, often referred to as multidirectional instability, means the shoulder capsule is inherently more elastic and less restrictive.
- Congenital Factors: The shape of the bones or the orientation of the glenoid socket may contribute to a less stable joint from birth.
- Connective Tissue Disorders: Systemic conditions like Ehlers-Danlos syndrome or Marfan syndrome can affect the quality and strength of collagen, the main component of ligaments and the joint capsule.
In atraumatic instability, the patient may not recall a specific injury. They often describe a feeling of the shoulder “slipping” or “going out” in multiple directions.
3. Neuromuscular Instability
While less common, problems with the nerves or muscles can also contribute to shoulder instability. The dynamic stabilizers rely on a healthy nervous system to fire correctly and at the right time.
- Rotator Cuff Dysfunction: Chronic tears or weakness in the rotator cuff muscles may leave the joint vulnerable. If the muscles cannot keep the humeral head centered, the joint can become unstable.
- Scapular Dyskinesis: This refers to an abnormal movement pattern of the shoulder blade. If the scapula does not move correctly, the socket is not positioned optimally to receive the humeral head.
- Nerve Injury: Damage to the nerves that supply the shoulder muscles may cause muscle weakness and atrophy.
The Patient’s Experience: Symptoms of Instability
Regardless of the underlying causes of shoulder instability, patients typically experience a range of symptoms that interfere with daily life and athletic performance.
- Dislocation: The most obvious symptom is a complete dislocation, where the joint pops out and stays out. This is typically intensely painful and requires medical attention to reduce the joint.
- Subluxation: This is a partial dislocation where the joint slips out and then spontaneously pops back in. Patients often describe a feeling of the shoulder “giving way” or a sudden, sharp pain followed by a dull ache.
- Apprehension: A feeling of fear or anxiety that the shoulder will dislocate when the arm is placed in certain positions.
- Chronic Pain and Aching: Over time, constant micro-movements and strain on the surrounding muscles may lead to persistent, dull pain, especially with activity.
Diagnosis: Pinpointing the Cause
A precise diagnosis helps guide the most appropriate treatment path. A physical exam includes specific tests to assess the stability of the joint in various directions. The doctor will check for generalized ligamentous laxity and perform tests to determine the direction of instability.
Imaging studies may also be used to support the diagnosis or for treatment planning:
- X-rays: Standard X-rays may be used to look for fractures, bony Bankart lesions, and Hill-Sachs lesions. They also help assess the overall alignment of the joint.
- Magnetic Resonance Imaging (MRI): An MRI is important for visualizing soft tissue injuries. It may show tears to the labrum, ligaments, and rotator cuff tendons.
- Computed Tomography (CT) Scan: A CT scan may be used to measure bone loss on the glenoid and the size of the Hill-Sachs lesion. This information is helpful for surgical planning.
Treatment Principles Based on Cause
The treatment strategy is always tailored to the specific cause of shoulder instability and the patient’s lifestyle. An experienced shoulder specialist can evaluate the condition and help guide the most appropriate treatment path.
Non-Operative Management
Non-operative treatment is the first line of defense for many cases instability.
- Physical Therapy: The focus is frequently on strengthening the dynamic stabilizers: the rotator cuff and the scapular muscles. The goal is to create a muscular “cuff” that can compensate for the underlying ligamentous laxity.
- Activity Modification: Avoiding positions that provoke instability may mean temporarily stopping overhead sports or modifying work activities.
- Anti-inflammatory Medication: Non-steroidal anti-inflammatory drugs (NSAIDs) can help manage pain and inflammation associated with chronic instability.
Surgical Management
Surgery may be recommended for recurrent traumatic instability, especially in young, active individuals, or when structural damage (like a large Bankart lesion or bone loss) is present.
- Arthroscopic Stabilization: For soft-tissue injuries like a Bankart lesion without significant bone loss, a minimally invasive arthroscopic procedure is often performed. The surgeon uses small instruments and a camera to reattach the torn labrum and tighten the stretched ligaments.
- Open Stabilization (Bone Grafting): When there is significant bone loss, a bone-grafting procedure, such as the Latarjet procedure, may be necessary. This involves transferring a piece of bone (the coracoid process) and its attached muscles to the front of the glenoid to reconstruct the missing bone and provide a muscular sling for added stability.
Summary
Shoulder instability happens when the shoulder becomes loose and the ball of the arm bone doesn’t stay securely in the socket. This can range from a “slipping” sensation to a full dislocation. It often starts after an injury, but it can also develop over time from repetitive overhead movements or naturally looser ligaments.
People may feel pain, weakness, or fear that the shoulder will “give out” in certain positions. A physical exam and imaging (like X-rays or MRI) help determine what’s causing the instability.
Treatment usually begins with physical therapy to strengthen the muscles that support the joint. If instability keeps returning, especially after an injury, surgery may be recommended to repair or tighten damaged structures. The goal is to restore stability, protect the joint, and help patients return to daily activities or sports safely.
Frequently Asked Questions
What is the difference between shoulder instability and a shoulder dislocation?
A shoulder dislocation is a single, acute event where the ball completely comes out of the socket. Shoulder instability is the chronic condition that results from the damage caused by the dislocation. Instability is the tendency for the shoulder to dislocate or subluxate repeatedly.
Can shoulder instability heal on its own without surgery?
It depends on the cause. Atraumatic instability, which is often due to loose ligaments, frequently responds well to intensive physical therapy aimed at strengthening the surrounding muscles. Traumatic instability, especially with significant labral tears or bone loss, may necessitate surgical intervention, particularly in young, active patients who face a high risk of recurrence.
How long does recovery take after surgery for shoulder instability?
Recovery is a multi-stage process. The arm is typically immobilized in a sling for several weeks to allow the repaired tissues to heal. Physical therapy then begins, focusing first on restoring range of motion and then on strengthening. Many patients can return to light daily activities within 6 to 8 weeks and can often return to competitive sports between 6 months and a year, depending on the complexity of the repair and the surgeon’s protocol.