Platelet-rich plasma (PRP) therapy has emerged as a promising treatment in orthopedic medicine, offering a regenerative treatment approach. Patients may seek this treatment for a variety of conditions, including chronic pain, injuries, and degenerative conditions. A common question for those considering the treatment is, “How long does PRP take to work?” The answer is not always straightforward, as the timeline for experiencing benefits can vary based on several factors, including the treated condition, individual health factors, and the specific PRP protocol used. In this post, we’ll provide a detailed overview of what patients may expect from PRP therapy.
Key Takeaways
- Platelet-rich plasma (PRP) uses a concentration of the patient’s own platelets, which are rich in growth factors, to help stimulate natural tissue repair.
- PRP offers a non-surgical, regenerative alternative for patients who have failed conservative care but wish to avoid invasive procedures.
- The injection is performed with precision to deliver the healing factors directly to the damaged plantar fascia tissue.
Understanding Plantar Fasciitis
The plantar fascia is a thick band of tissue that runs across the bottom of your foot, connecting your heel bone to your toes. It acts like a shock absorber, supporting the arch of your foot. When this band becomes inflamed, irritated, or, more commonly, degenerated, the resulting condition is known as plantar fasciitis. A common symptom is intense, sharp pain near the heel, especially when you first stand up after sleeping or resting. The pain often lessens after a few minutes of walking but may return after long periods of standing or activity.

Who is at Risk?
Several factors may increase a person’s risk of developing this painful condition:
- Being overweight or obese, which can place added stress on the plantar fascia
- Having high arches, flat feet, or other biomechanical foot issues
- Working in jobs that require prolonged standing
- Participating in high-impact activities like running or certain sports
Age also plays a role, with the condition being most common in people between 40 and 60 years old.
Traditional Treatment Pathways
Initial treatment strategies generally focus on rest and reducing the mechanical stress on the foot. Patients often begin with simple measures they can perform at home.
- Rest and Ice: Reducing activities that aggravate the pain and applying ice to the affected area may help manage discomfort.
- Stretching and Physical Therapy: Specific exercises to stretch the plantar fascia and the Achilles tendon may be key parts of recovery. A physical therapist can provide a tailored program.
- Supportive Footwear and Orthotics: Wearing shoes with good arch support and cushioning may help in many cases. Custom or over-the-counter orthotic inserts can distribute pressure more evenly across the foot.
- Night Splints: These devices hold the foot in a slightly flexed position while sleeping.
When Conservative Care Fails
Most patients find relief within several months of consistent conservative care. However, for some patients, the pain becomes chronic, lasting longer despite diligent treatment.
Historically, one of the most common next steps was a corticosteroid injection. Corticosteroids are powerful anti-inflammatory agents that can provide rapid, significant pain relief. However, they do not promote tissue healing. Additionally, repeated corticosteroid injections may potentially weaken the plantar fascia tissue over time.
Regenerative Medicine: The Power of PRP
Regenerative medicine focuses on stimulating the body’s natural ability to heal itself. Platelet-rich plasma, or PRP, is an example of this approach in orthopedic care.
PRP is a concentration of platelets derived from the patient’s own blood. Blood is composed of red blood cells, white blood cells, plasma, and platelets. Platelets are best known for their role in clotting, but they also contain hundreds of proteins called growth factors. These growth factors support healing. When concentrated and injected into an injured area, they may help initiate and accelerate the body’s repair process.
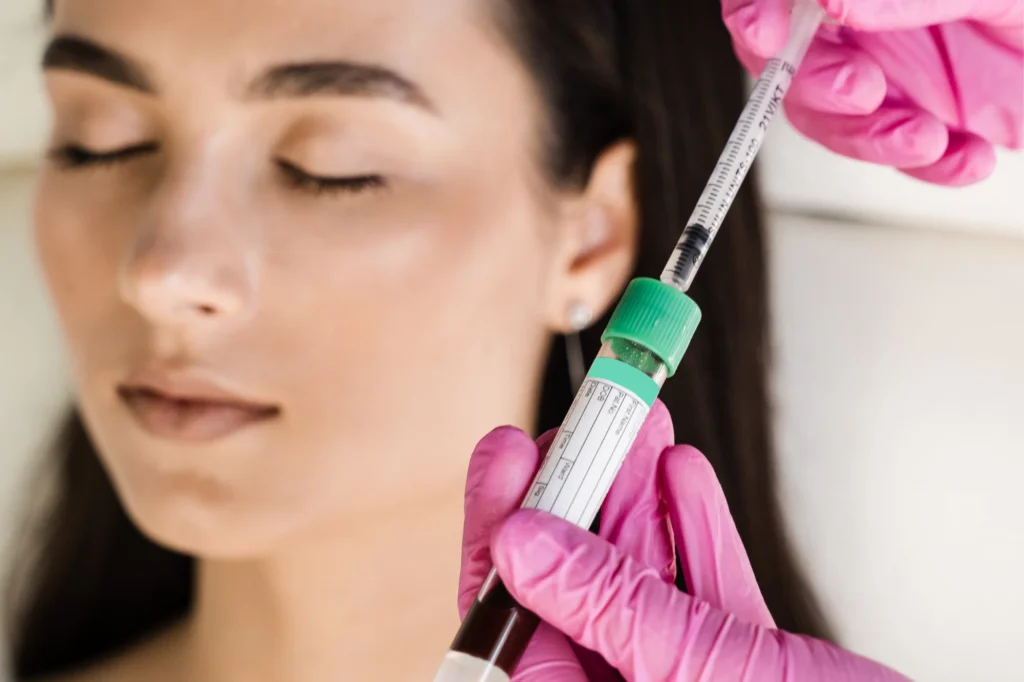
What to Expect from PRP Injections for Plantar Fasciitis
The process of receiving a PRP injection is straightforward and can be completed in an outpatient setting, typically taking less than an hour.
Pre-Procedure Preparation
Patients are generally advised to stop taking non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen, for one to two weeks before the procedure. These medications may interfere with the function of the platelets, potentially reducing the effectiveness of the PRP. Patients should also maintain good hydration ahead of their appointment.
The Three-Step Process
The PRP therapy procedure involves three main steps: blood collection, platelet concentration, and injection.
Step 1: Blood Collection
Blood is taken from the patient’s arm in a process similar to a standard lab test. The volume of blood collected depends on the specific PRP system used and the area being treated.
Step 2: Centrifugation
The collected blood is placed into a specialized centrifuge machine. This device spins the blood at high speeds, separating its components based on density. This process isolates the red blood cells, the platelet-poor plasma, and the layer containing the concentrated platelets and white blood cells. The physician then extracts the platelet-rich layer, which now contains a platelet count several times higher than that found in normal blood.
Step 3: The Injection
Your doctor may use an ultrasound machine to visualize the plantar fascia and the exact location of the degeneration or tear. This imaging guidance ensures that the concentrated PRP is delivered precisely to the area of damaged tissue. While the injection of the PRP solution may cause a temporary feeling of pressure or fullness, the procedure is minimally invasive and generally well-tolerated.
Recovery and Rehabilitation
Unlike some treatments that require immediate immobilization, the focus here is usually on a gradual return to activity, allowing the regenerative process to take hold.
Immediate Post-Injection Care
Patients typically experience some soreness, swelling, and tenderness at the injection site for the first few days. This is a normal and expected response. Ice may help to keep the pain manageable. It is important to remember that patients should often continue to avoid NSAIDs during this initial period, as these medications can counteract the healing process that the PRP is designed to stimulate.
Activity Modification
For the first week, patients are generally advised to limit weight-bearing activities. High-impact activities, such as running or jumping, are typically restricted for several weeks to a few months, depending on the patient’s specific response and your doctor’s protocol. The goal is to protect the newly forming tissue while still promoting healthy movement.
The Role of Physical Therapy
Physical therapy is frequently an important component of the recovery process after receiving PRP injections for plantar fasciitis. Once the initial soreness subsides, a structured physical therapy program can help to restore flexibility, strengthen the foot and ankle, and improve overall biomechanics.
Timeline for Results
PRP is a regenerative therapy, and tissue healing takes time. Unlike a corticosteroid injection, which can offer immediate but temporary relief, PRP tends to work gradually. Patients often begin to notice a reduction in pain and an improvement in function within two to six weeks. The most significant improvements typically occur over a period of two to three months, and the healing process may continue for up to six months or, in some cases, longer.
Summary
Plantar fasciitis is a complex condition that can transition from a simple inflammation to a chronic degenerative state. PRP is a regenerative treatment option that utilizes the patient’s own concentrated growth factors to stimulate tissue repair. The procedure is minimally invasive, and, especially when combined with a dedicated physical therapy program, may support sustained improvements in both pain and function. Consulting with an experienced orthopedic specialist is the first step to determine if this regenerative therapy is the right choice for your chronic heel pain.
Frequently Asked Questions
How many PRP injections will I need for plantar fasciitis?
In some cases of long-standing chronic fasciitis, a second injection may be considered. Your doctor will evaluate your progress after the initial treatment to determine if a booster injection is recommended.
How long after the PRP injection can I return to running or sports?
A gradual return to high-impact activities helps protect the healing tissue. Many patients are advised to avoid running and strenuous sports for at least six weeks. The exact timeline depends on your pain level, the severity of your initial condition, and your progress in physical therapy. Always follow the specific guidance provided by your orthopedic specialist.
Do I need to stop all my medications before the procedure?
Patients are generally recommended to stop taking non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen, naproxen, and aspirin for one to two weeks before the procedure. These medications may interfere with platelet function. You should discuss all your current medications, including supplements, with your physician during your consultation.